Our New Analysis of Myocarditis after Vaccination: Combining 85 year old women with 20 year old men is Bad Medicine
Young men need different advice than old women
One raging debate during the pandemic has been whether, and under what circumstances, the risks of mRNA vaccination exceed the risks of the virus. Of course, for an 80 year old who had not had COVID19 as of Jan 2021, the net benefit of vaccination was clear. RCTs had shown a reduction in severe disease, and this was definitely orders of magnitude bigger than any adverse events hitherto unknown. (It had to be due to basic math)
However, the calculus was different for a 16 year old boy who already had 1 dose of Moderna. On day 28, he has a choice, get dose 2 and then, eventually get COVID19, or just get COVID19. The first dose already dramatically reduced his risk of bad COVID19 outcomes, and the second dose carries the greatest risk of myocarditis. Either way he gets COVID19 eventually. Which pathway is best? Or perhaps there could be a middle path: delay dose 2 or lower the dose?
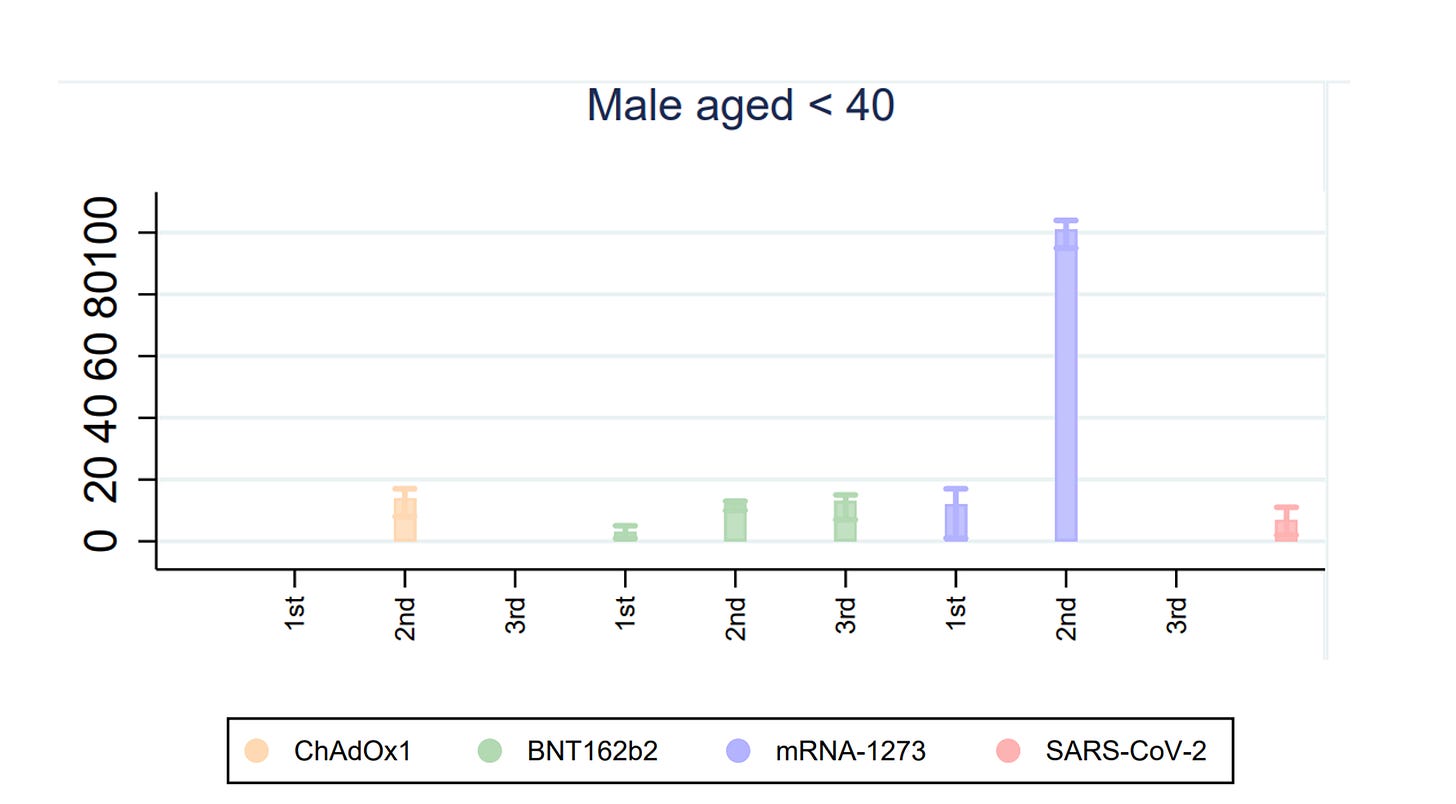
Of course, I analyzed this question and related ones throughout the pandemic. As early as July 2021, with colleagues from mathematics, cardiology, and pediatrics, we worried that dose 2 was unfavorable in adolescent boys. With emerging data from the UK it was clear that for some products and some doses, myocarditis post vax exceeded myocarditis post illness. See pic.
And yet, COVID19 influencers— with no ability to analyze data— continued to make the false statement that COVID19 had worse myocarditis under all circumstances. They blindly pushed their anti-anti-vax zealotry. Yet, you can see clearly (above) that was not true. (PS the red bar is exaggerated because the denominator was not sero-prevalence based but documented test based)
Enter our new peer-reviewed analysis now out in EJCI.
In our paper, we prove something interesting. If you look at all the analyses of myocarditis post vaccine, some researchers breakdown results by age, sex, product and dose. (4 stratifiers), while others lump 20 year old men with 80 year old women (<=1 stratifier). And many inbetween.
It turns out when you look at myocarditis just in the highest risk demographics it is substantially higher than when you lump 16 year old boys with their great grandma.
This should be obvious, but was habitually done by mRNA myocarditis minimizers to hide the safety signal, and let CDC and FDA fail to take appropriate safeguards like testing lower doses, longer spacing, banning Moderna, or omitting dose 2 entirely. This same hubris led to incorrect policies around booster mandates in young men, a topic we have published a separate peer review paper on.
Our analysis is full of interesting findings. Dose 2 is worse than dose 1. Moderna is worse than Pfizer, Dose 2 is a big problem, and more. But these differences are lost in analyses that lump together products or combine young men and old women.
Recently, the cardiologist Eric Topol, who in my estimation frequently provides poor and incorrect analyses on many topics, tweeted this claim. Here, he mades this exact error.
He combines 5 year olds with 25 year olds. Of course, it was well known myocarditis post vaccine is largely a post pubescent phenomenon. He combines 20 year olds with 39 year olds. As someone on the upper end of that range, let me assure you, I wish I were 20. He also combines men and women. Hard to believe, but that is the statistic he highlighted.
And his take home is incorrect. Myocarditis is a salient concern for men 12-35, and greatest 16-26. These young men need different guidance than an 85 year old woman. Or even a 39 year old man. They don’t need to be reassured that its better than covid, because the purpose of medicine is to shield them from preventable drug toxicity.
Our analysis is the first to prove that one can minimize mRNA myocarditis by failing to break it out by basic demographics. This was a common error sadly during the pandemic. Please read and share our paper. I think you will find the discussion fair and balanced.
Sensible medicine means that it is ok to acknowledge that all medical products have benefits and risks, and these can vary depending on the age and sex. A 20 year old man needs different guidance, and probably should not get an annual booster, while an 85 year old woman in a nursing home probably should. Both groups need more randomized data.
This is not a controversial take; it is medicine 101, but was forgotten by so many (CDC & FDA) who were tasked with protecting young men due to ignorance or political expedience.







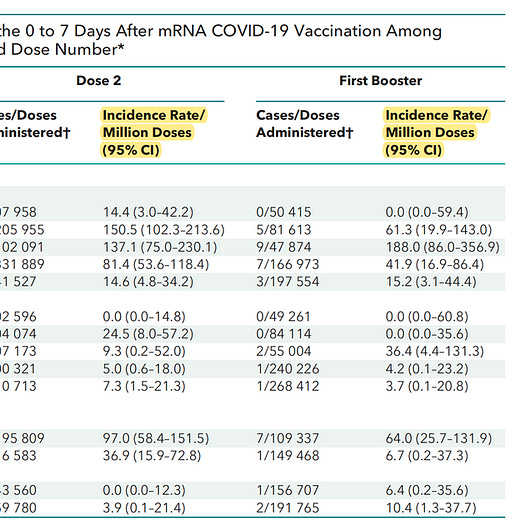
Nice paper -- but not a single surprising finding. Most of us have known this since the beginning...really, the signals have been there all along if one looked. Thrilled to have it laid out in a more rigorous fashion that, while not unexpected, is pretty unassailable.
And it is clearly politics, not ignorance, that has driven this entire conversation for several years. Topol (whom I have come up against several times -- all unpleasantly) will say anything he thinks will advance his career. There is not a scientific bone in his body. It is an embarrassment that he puts himself forth as a knowing doctor. There are a handful like this that have captivated the government-endorsed-doctor-pool...shameful. I cannot wait until they are replaced by real doctors and real scientists who are driven by patient care, not politics.
Thank you for adding one more brick to the foundation to send these people away. And amnesty is NOT in my vocabulary these days. These have all been bad actors for reasons unrelated to health and health care, sadly.
It’s crazy to me as a pediatrician. The big cliche we constantly hear in training, from med school through residency, is “children are not little adults.” Yet Covid comes along and the AAP and mindless majorities of pediatricians treat children… like little adults. Madness!
P.s. your analysis above also reminds me of the infamous leaked “hide the decline” emails from the global warming researchers a few years back. You can’t come up with the results you need to panic the population (and increase your funding) without deliberately manipulating the figures. It’s a clear sign of a guilty conscience. These people aren’t just wrong, they’re malicious.
https://gaty.substack.com/